Public & Private Insurance
- Know the Policy
- Know the Process for Obtaining AT
- Coordinate Insurance and Other Benefits
- Appeal Denials
Private insurance is any health insurance policy purchased by an employer or by an individual from a private insurance company.
Public insurance is an insurance plan or policy that is subsidized by federal or state funds (Medicaid, Medicare). To be eligible for these plans an individual must meet one or more qualifying criteria involving age, income level, and health status.
Throughout this section, we will be discussing both public and private insurances. Insurance coverage goes by different names: we will refer to private insurance as an insurance policy. Medicaid coverage is dictated by a State Plan, and Medicare coverage is determined by national Medicare Policy. For simplicity in this section, we will refer to all three as a “policy.”
Individuals may be covered by a single insurance policy or by multiple policies. While there is considerable variability among what health insurance companies and state and federal plans cover with regard to AT, keep these general considerations in mind when dealing with public and private insurance.
Private insurance is often overlooked when efforts are made to obtain AT for persons with disabilities. If one has private insurance, Medicare and Medicaid consider that insurance to be the "payor of first resort," and will not consider funding requests until an individual's private insurance has denied all or part of the claim. There are three main questions when one looks to any insurance to fund AT:
- Is the child or adult with disabilities covered by the policy?
- Is the AT being sought covered by the policy?
- Is the AT medically necessary?
Know the Policy
- Know the type of policy. For example, in a fee-for-service plan, the provider submits a bill to the payer after the service or equipment is provided. In the case of managed care plans, decisions about paying for services or equipment are generally made before the service or equipment is provided.
- Remember that AT is referred to in some insurance policies by other names, such as durable medical equipment (DME), home medical equipment, rehabilitation technology, orthopedic appliances, medical supplies, vision services and equipment, or prosthetic devices. Stay alert to any policy changes that might improve coverage.
- Read the insurance policy, certificate of coverage and accompanying documents carefully so that you understand the policy's definitions, covered benefits, exclusions, deductibles, caps, etc. Make sure you obtain the actual contract and not just a handbook or summary. DME is usually not available in a "basic" plan but rather in a "major medical" plan, which is often a rider to a basic plan. Be aware not only of exclusions for certain types of DME but also of clauses that limit the dollar amount of funding for a particular item.
- Be aware that an AT device can sometimes be provided as part of therapy services even if not explicitly listed as a covered AT device. For example, one might be able to obtain an augmentative and alternative communication (AAC) device as a component of covered speech and language therapy services.
Know the Process for Obtaining AT
- Health insurance will pay for AT if it meets that insurance policy's particular definition of AT (by whatever name it's known) and if the request meets that policy's criteria for "medical necessity." The definition of "medical necessity" generally means that: (a) the device is prescribed by a physician; (b) it is used to restore or approximate normal function of a missing, malformed, or malfunctioning body part; (c) the device is directly related to a diagnosed medical condition; and (d) the device is expected to improve the user's ability to function. Keep in mind that this is how medical necessity is generally defined; consult the insurance policy for specific guidelines.
- Most health insurance policies require prior approval for AT. Look to the insurance policy's benefits booklet for a description of the required procedure.
- Follow the policy's process for acquiring AT. In addition to the doctor's prescription, this may include supporting documentation from other health care providers and therapists (speech/language, occupational, physical) regarding "medical necessity" and the expected benefits from the AT device or service. Refer to—and even incorporate—the language stated in the policy when writing supporting letters.
- Understand the method of payment accepted by the AT supplier.
- Find out whether the AT supplier will file the claims paperwork to request payment or whether that will be the responsibility of the insured party or a service provider.
Coordinate Insurance and Other Benefits
- Identify all potential payment sources for which an individual is eligible before applying to any. Make sure you understand whether there is an order in which the sources must be tapped. For example, one must always exhaust private insurance payment options before applying for Medicare or Medicaid payment, and Medicaid will require someone dually eligible for Medicare and Medicaid to make application to Medicare first.
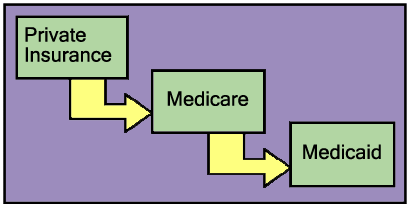
- Medicaid is considered the "payor of last resort" in most cases. The exception to this rule is when the device and/or service is both medically and educationally necessary for a child. In such cases, Medicaid functions as the "payor of first resort."
- If you anticipate combining resources from several payors to fund devices and services, you will need to make sure that all of the payors include your selected service providers/equipment vendors among their authorized providers. It is not unusual for a private insurance company to exclude a provider that Medicaid includes on its list of approved providers. If you fail to consider this in advance, you can find yourself being denied access to a service or device simply because you started the process with a provider that was not enrolled with (authorized by) all insurance plans.
Appeal Denials
- Unfortunately, denials are often the rule rather than the exception when it comes to seeking payment for AT. Consider the denial to be a request for more information. Do not assume that the insurance plan properly interpreted its own eligibility and coverage rules. Review the relevant language of these rules yourself.
- Insurance providers are required to provide a written notice of denial. Once you have a written denial on an Explanation of Benefits (EOB) or other form, check your policy coverage guidelines for information about appeal procedures. Take advantage of any opportunity to discuss the decision by phone with the insurance provider.
- Follow the appeal procedures, paying careful attention to time limits. Supply any additional evidence from your physician or others that will support your claim. Be prepared to argue, if appropriate, that the AT device is a necessary part of some therapy services or that it fits the policy's covered equipment definition even if not explicitly listed as covered equipment.
